Measles in Children – What You Need to Know
Article Table of Contents
From early 2024 to the present, the number of measles cases has increased compared to the same period in 2023 and continues to rise in several localities. On August 27, 2024, the People’s Committee of Ho Chi Minh City officially declared a measles outbreak, classified as a Group B infectious disease, across the entire city.
The public is advised to regularly update information on the epidemic situation, proactively take children for full and timely vaccination in accordance with the Ministry of Health’s guidelines, and implement preventive measures such as avoiding crowded gatherings, washing hands frequently with soap, and wearing face masks when visiting public places or crowded areas.
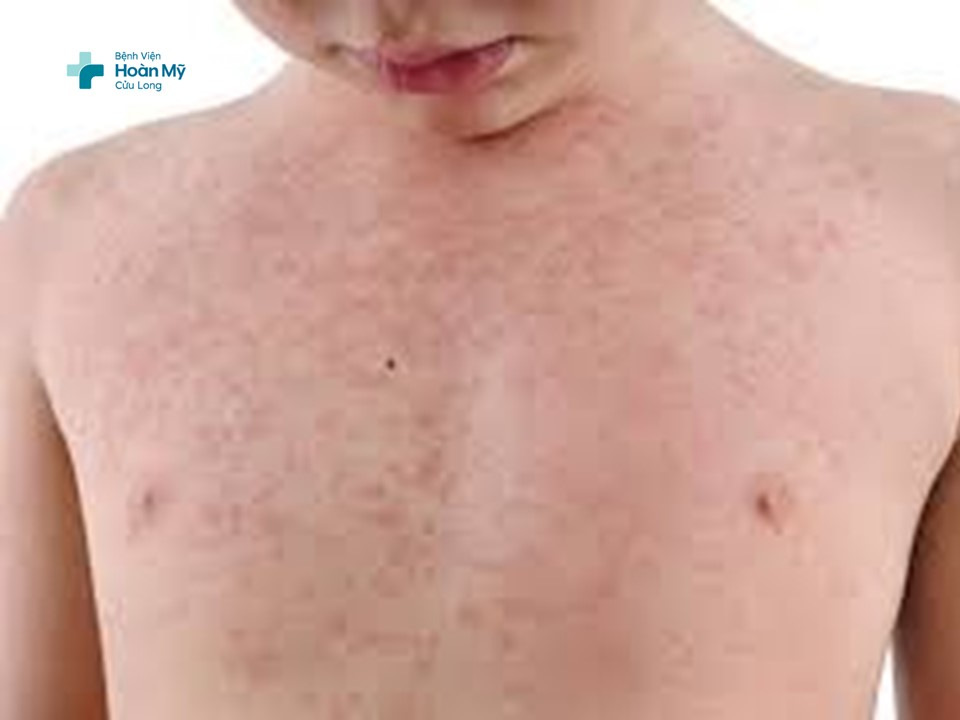
What is measles?
Measles is a highly contagious infectious disease transmitted via the respiratory tract and caused by the measles virus. It primarily affects children under five years of age and often occurs during the winter–spring season. Adults may also be affected if they have not been vaccinated or have not completed the full vaccination schedule. The disease spreads rapidly and can cause outbreaks.
Typical symptoms include fever, upper respiratory catarrh, conjunctivitis, and rash. Measles can lead to serious complications such as pneumonia, encephalitis, otitis media, corneal ulceration, diarrhea, and may be fatal.
How is measles transmitted?
Measles is mainly transmitted through the respiratory route. It spreads particularly quickly in community settings such as schools, daycare centers, and kindergartens if infected children are not isolated.
Signs and stages of measles
Typical form – four stages
- Incubation period: 7–21 days (average 10 days) after exposure to an infected person.
- Prodromal stage (catarrhal stage): Lasts 2–4 days. Children develop high fever, cough, runny nose, and conjunctivitis. Acute laryngitis may occur. Koplik spots may be observed – small (0.5–1 mm), white/gray lesions with a red halo on the buccal mucosa opposite the upper molars.
- Rash stage: Lasts 2–5 days. After 3–4 days of continuous high fever, a maculopapular rash appears. The rash blanches on pressure and starts behind the ears, at the hairline, forehead, face, and neck, then spreads to the trunk and limbs, including the palms and soles. When the rash spreads throughout the body, the temperature gradually decreases. The lesions may merge into large patches.
- Recovery stage: The rash fades, turns grayish, peels with fine scaling, leaving temporary hyperpigmented “tiger-skin” streaks, and disappears in the same order as it appeared. Without complications, the disease resolves spontaneously. A cough may persist for 1–2 weeks after the rash subsides.
Atypical forms
- Mild fever, mild cough and runny nose, few rashes, and good general condition. This form is easily overlooked, leading to unrecognized transmission.
- Severe form with persistent high fever, atypical rash, limb edema, generalized pain, often accompanied by severe pneumonia.
Complications of measles in children
Severe measles and its complications are more common in malnourished children, especially those with vitamin A deficiency or immunodeficiency due to HIV infection. Most deaths from measles in children are caused by complications.
- Due to the measles virus: giant cell interstitial pneumonia, laryngotracheobronchitis, myocarditis, encephalitis, and acute meningitis.
- Due to secondary infections: pneumonia, otitis media, gastroenteritis, etc.
- Due to poor nutritional status and inadequate care: necrotizing stomatitis (noma), corneal ulceration leading to blindness, malnutrition, etc.
- Other complications: progressive tuberculosis and diarrhea.
In pregnant women, measles infection may result in miscarriage, stillbirth, preterm birth, low birth weight, or congenital measles infection in the newborn.
How is measles diagnosed?
Laboratory tests
- Basic tests: complete blood count, chest X-ray
- Measles virus detection:
- Serology: blood sample from day 3 after rash onset to detect IgM antibodies
- RT-PCR or viral isolation from blood or nasopharyngeal specimens in early stages (if available)
Diagnostic criteria
Diagnosis is based on:
- Epidemiological factors: contact with measles patients or multiple cases in the family/community
- Clinical features: fever, cough, catarrhal symptoms (respiratory, conjunctival, gastrointestinal), Koplik spots, and characteristic rash
- Laboratory confirmation: presence of measles-specific IgM antibodies
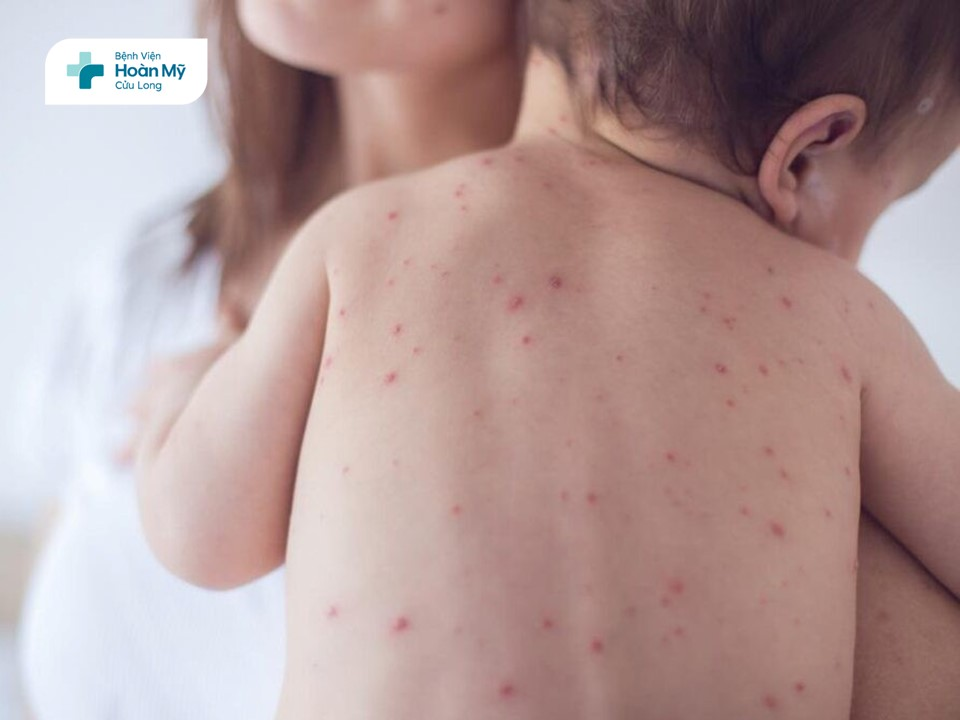
Differential diagnosis
Measles should be distinguished from:
- Rubella: rash without progression pattern, rare catarrh, cervical lymphadenopathy
- Enterovirus infection: non-sequential rash, often vesicular, associated with gastrointestinal symptoms
- Kawasaki disease: persistent high fever, red lips and tongue, cervical lymphadenopathy, non-sequential rash
- Other viral exanthems
- Allergic rash: itching, eosinophilia
Treatment
Principles
- No specific antiviral treatment; management is supportive
- Isolation of patients
- Early detection and treatment of complications
- Do not use corticosteroids unless measles has been ruled out
Supportive care
- Hygiene of skin, eyes, mouth, and throat (avoid corticosteroid-containing products)
- Adequate nutrition
- Fever control:
- Physical cooling (lukewarm sponging, cool compresses)
- Paracetamol for high fever
- Oral rehydration; IV fluids only if severe vomiting or risk of dehydration/electrolyte imbalance
- Vitamin A supplementation
Treatment of complications if present (pneumonia, diarrhea, conjunctivitis, etc.)
Measles prevention
Non-specific prevention
- Early detection and isolation of suspected or confirmed measles cases.
- Measles patients must be isolated at home or at healthcare facilities in accordance with respiratory infection control principles.
- Surgical masks should be used by patients, caregivers, close contacts, and healthcare workers.
- Limit unnecessary close contact between healthcare workers, visitors, and patients.
- Isolation should be maintained from the time measles is suspected until at least 4 days after the onset of rash.
- Strengthen personal hygiene, disinfect the nose and throat, keep the body warm, and improve overall physical condition to enhance immunity.
- Prevent hospital-acquired transmission.
Active prevention with vaccination
- Administer two doses of measles vaccine to children according to the National Expanded Program on Immunization (the first dose is mandatory at 9 months of age).
- Provide measles vaccination to other eligible groups as guided by health authorities.
Infection prevention in healthcare facilities
- Strictly isolate suspected, probable, and confirmed cases.
- Comply with infection control and transmission prevention measures for healthcare workers, caregivers, and other patients in accordance with Ministry of Health guidelines.
Article by: Dr. Pham Nguyen Yen Trang, MD, CKII – Deputy Head of Pediatrics Department, Hoan My Cuu Long Hospital.
Share
Hoan My Hospital Network
-
Hoan My Cuu Long HospitalAddress: Lot 20, Vo Nguyen Giap Street (Quang Trung), Phu Thu Ward, Can Tho City
phone: 0292 3917 355
email: [email protected]